Resource Details
Resource Format
Categories
Share:
Some medical practices and hospitals have family support clinicians or clinical social workers that can help patients with sensory needs or communication impairments identify support services within the community. Family support clinicians make referrals, collaborate, problem-solve, and connect to supports to help autistic adults and caregivers successfully navigate services across the lifespan. These “wraparound services” address important needs across the lifespan like medical/health concerns, special education, social/behavioral supports, public benefits, legal/financial advice, housing, vocational training, transportation, etc.
Not every medical practice serving adults has a support clinician, but caregivers and self-advocates can encourage the practice to create such a resource. Support clinicians not only improve the lives of autistic adults and their caregivers, but they also ease the workload of the entire practice by ensuring whole-life health for all patients and their caregivers.
Julie M. O’Brien, MEd, LMHC, a Family Support Clinician at the MGH Lurie Center for Autism, helps to educate and support families by identifying a range of home- and community-based supports and resources by age and stage of life. She serves as the liaison between the patients’ provider and parents/guardians/families, and points them in the right direction.
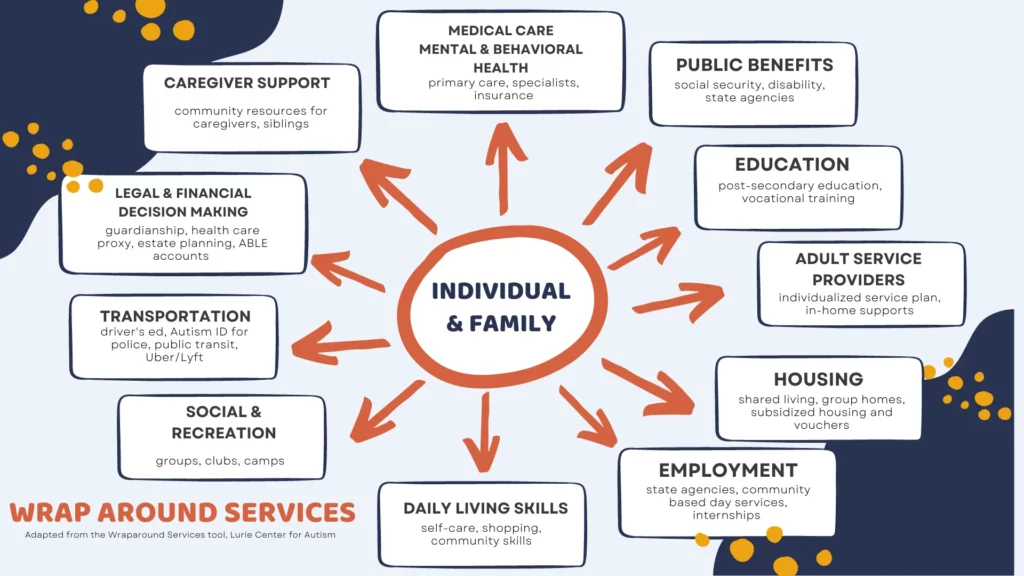
Useful links to find out more about sites and organizations that can help with wraparound services.
Housing
Education
Independent Living and Life Planning
Employment
Service Providers
Legal & Financial Issues
Social Connections & Supports
Support for Families of Those with Profound Autism

More Resources
Find more information on legal considerations, navigating insurance, tools for managing information, and other key topics.





